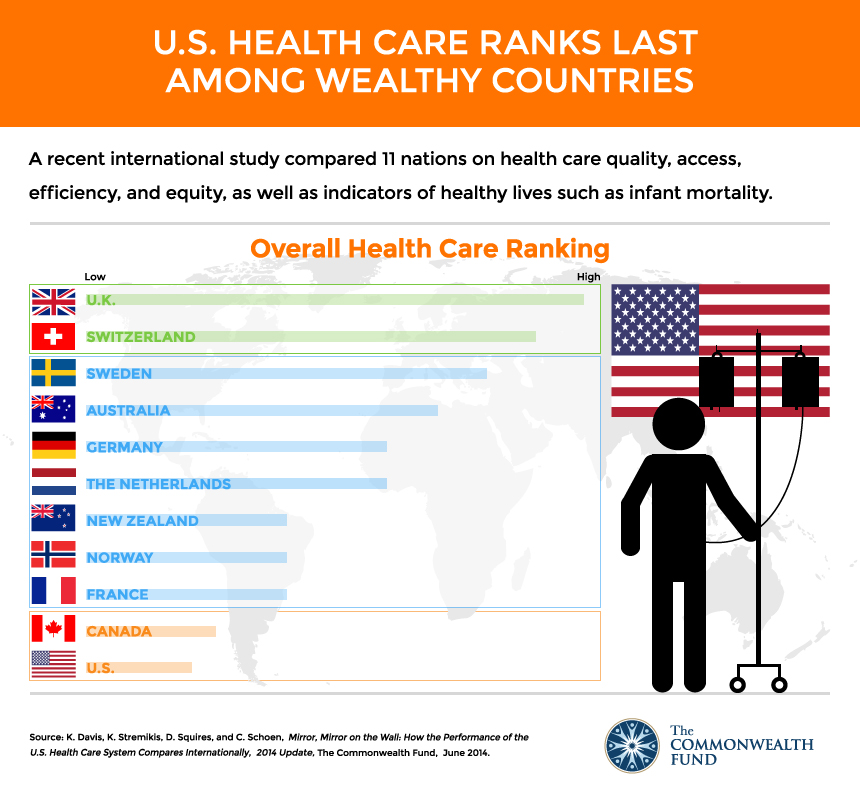
The UK and the US health care services are great examples of publicly funded and privately funded health care systems respectively. By assessing and analysing key findings from a microeconomic standpoint, we can see significant difference between the two approaches to health care provision.
First, the role of government interventions in the provision of healthcare is to balance the demand and supply of the services; as well as prevent market failures in the form of monopoly, price fixing, and exploitation. Insurance system is also introduced to avoid information asymmetry in the market. We then look into the UK health care service and see that a public funded system will attempt to discourage market failures by avoiding information asymmetry, negative externalities and regional monopolies. However, the National Health Service (NHS) suffers from allocation and productive inefficiencies. The US system benefits from a competitive market model, this having higher levels of economic efficiency, innovation and quality of service. On the other hand, the US model is often criticised for not offering equal welfare to society, in addition, it leads to waste and the dominance of insurance companies. Finally, we will assess the role of a regulator when ensuring efficiency and competitiveness as well as discouraging market failures; whereas the role of a market form will ensure better allocative efficiency in healthcare provision.
Introduction
In the UK, the NHS has existed for over fifty years and offers health care that is free at the point of delivery for everyone. This service is funded by taxpayers for the benefit of those same taxpayers. However, the option remains available for people to purchase private health insurance if they so choose.
In the US, the majority of citizens have health insurance that is related to employment or purchases directly. The federal government only ensures public access to emergency services, regardless of an individual’s ability to pay. They also have publicly funded health care programs that cater to the elderly, the disabled and the poor.
These are two significant examples of the two different approaches to health care provision: publicly and privately funded. In this report, we are going to look into the microeconomic aspects of the two models by assessing and analysing:
- Health care features as policy interventions in the market
- The microeconomic advantages and disadvantages of the UK system
- The microeconomic advantages and disadvantages of the US system
- The role of the regulators and markets in the provision of health care
Key Findings
Health care features as policy interventions in the market
In the majority of advanced societies, access to basic and emergency health care is considered an irrefutable moral right, regardless of gender, age or creed. But through what means should a government decide it has the right to control any health care system via administration and policy? Both systems contain state owned entities which provide free health services, funded by the taxpayer, although the limitations on state services differ greatly, defining the private and public services. By its very nature, a state owned entity requires policy interventions in its administration, in order to decide what services each government chooses to provide.
As a nationalised service, both UK and US government run monopolies on health care on some level. At the same time, medical institutions such as hospitals may create localised monopolies since no other alternative may offer their services and economies of scale incentivise ‘the emergence of one large hospital in an area rather than a large number of small hospitals’. By definition, monopolies create economic inefficiencies through social loss such that a monopoly firm may retain higher profits from their personal gain. Where health care exists as a privately provided system, the same regulations and policies that are inflicted on all free enterprise may be used. Such policies exist to ensure perfect competition where possible, to prevent the formation of cartels or price fixing, and to limit the exploitation and advantages given to any natural monopoly.
With free service, demand for health care from the common citizen is at its practical maximum. The role of government is to supply this demand to the best of its ability. Such, it can be seen that the government itself has a demand for a level of health care which creates an equilibrium against what the production firms can supply. Policy intervention is therefore required to choose the appropriate level of demand the government wishes to obtain, given the cost of supply, the health demands of the people and the level of funding from taxes.
As the demand for health care is not a constant for any individual consumer, since accidents are unpredictable, a system of insurance has been adopted in many markets, whereby a prepayment to a firm is made, such that when demand for medical care is required, all costs are covered by the firm. The free health market funded by taxes may act as a proxy to an insurance system since taxes are paid regularly in exchange for returns via public services. With any insurance system, problems may arise if contracts are improperly defined or information is asymmetric, such that consumers are refused service if they are not adequately covered, or are unaware of the full extent of their insurance coverage. A policy and regulatory body may be necessary in order to ensure fair contracts are held without exploitation.

Advantages
Health care is a complex, unique good and everybody demand it but it faces problems if it is distributed through a free-market system and not a state-funded system. Market failure can occur for many reasons and the problem of asymmetric information is one of these. This is when producers and consumers within a market have access to different levels of information, whereas a characteristic of a completely competitive market is when all economic agents have access to all information. This is the case between doctors and patients as patients have minimal information (individuals cannot treat themselves). They expect doctors to act in their best interests but this may not happen in a free market. A doctor working for a company motivated by profit may act in the best economical interests of the company when deciding how to treat a patient.
Other causes of market failure include externalities and the forming of regional monopolies. These problems do not exist in a state-funded health care system and neither do insurance related problems.
‘The main aim of the NHS is to provide a comprehensive, high quality service available on the basis of clinical need and not ability to pay’. It is also a huge job provider, increases the productivity of the economy by keeping the workforce healthy (including preventative treatments like vaccinations) and increases real GDP by raising life expectancy and therefore lengthening the average working life (Riley, 2006).
The NHS also benefits extensively from economies of scale because of its size and is good value ‘at a total cost of around 6% of the GDP’, compared with 16% of the GDP for the US (Team project guidelines).
Disadvantages
Since profit is not the main incentive behind the NHS, and prices do not play the same role as in a free market system, inefficiencies exist. The power of a competitive market suggests that the correct quantity and quality of health care would be provided at minimal cost to meet consumer demand. This would not be the case for the NHS. The distribution of resources would not produce a Pareto efficient outcome.
Demand for health care simply outstrips supply and demand will continue to grow because of ‘changes in the age structure, increasing real incomes, improvements in medical technology’ (Office of Health Economics, 2009). As the population of the UK ages, the larger number of older people will put a greater strain on the NHS, increasing real incomes cause people to raise their standards and medical developments simply increase the number of conditions that can be treated. Government expenditure on health care will therefore need to increase or health care will have to be rationed to a greater extent.
The economics advantage and disadvantage of the US system
Advantages
Health care in the US is provided by many separate legal entities both in the private sector and public sector. This is a contestable market (or free market system) where anyone, any unions, any groups, regardless public or private, can provide health care. Hence, it increases the competitive level of health care provision to consumers, increasing economic efficiency. In addition, contestable markets also rule out the chance of monopoly rule and in doing so, prevents deadweight loss to the customers. In order to stay in the market, each entity needs to maximize quality of products (insurance, drugs price, medical fees) and minimize the costs. The contestability system opens up many opportunities for businesses which allow more research about drugs and health technology which will help cost saving in medicine. Furthermore, the US has some of the best medical research systems such as the Harvard Medical School, Mayo Clinic and the Cleveland Clinic.
Disadvantages
In an article discussing the US health care crisis, Paul Krugman and Robin Wells state that the US health system favours the wealthy especially the employer (Krugman & Wells, 2006). Whereas those with higher incomes pay medical fees using pre-tax income, some firms and wealthy people get a ‘tax-break’ in the form of access to all medical services available. For example, instead of paying the tax, some corporations pay the health insurance for their employees instead.
Furthermore, Paul and Robin also argue on the heavy reliance of the Americans on health insurance which leads to waste and the domination of the insurance companies (Krugman & Wells, 2006). As of 2008, private health insurance paid for 33.5% of the total spent on health expenditures account while out-of-pocket-payments consists of only 11.9% (Centers for Medicare & Medicaid Services, 2008). As health insurance in the US is mostly distributed by the private sector (67.5% in 2007) (Centers for Medicare & Medicaid Services, 2008), many people lack health insurance. This leads to a portion of Americans who have no jobs, have no insurance and hence they are not able to get any medical services. As of 2007, there is at least 15.3% of Americans who have no insurance (Centers for Medicare & Medicaid Services, 2008).
This system helps both the government and the consumers by creating greater savings on health services. Because the government is not the only one who provides health care, the government’s share in health care should be lower compared to economies where the government provides full services to all citizens. Also, as stated above, advances in technology that reduce cost in drugs production also benefit the public sector. In 2008, the US government only accounted for 47.3% (or $1.1 trillion) in the $2.3 trillion spent on health care services and products (Centers for Medicare & Medicaid Services, 2008).
The US health care seems to favour private business over public services. However, it also creates jobs and saves money for its customers which could lead to an increase in average disposable income.
The role of a regulator and markets in the provision of health care
Health care is a good that is, generally, under-supplied and over-priced in competitive markets. The role of the government, with regards to health care, should be to sustain supply at an optimal level that would not otherwise exist in a competitive market. Therefore, given this supply of health care provided by the government, regulators should exist to ensure the efficient operation of the NHS in the UK. Due to the lack of direct competition to the NHS, supply is only a function of costs, rather than being a function of price as well as costs, only because it is provided for free to consumers who demand it. In the US, where competitive markets determine the price and quantity of health care provided, there are high fixed costs in terms of capital and equipment and that those that supply health care engage in discriminatory prices as a result of the existence of market power (Glied, 2003). Shelly Glied notes that ‘[t]hese patterns suggested that per unit costs of health care could be reduced’ (Glied, 2003). Therefore, regulators should also act to ensure the competitiveness of the entire health care market in the US and the private health market sector in the UK.
The role of markets is to, by incentivising individuals to respond to signals in the market, achieve efficiency and equity in the health care industry (Le Grand, 1998). In order to maximise the supply of health care services, maximising efficiency should be the priority role for both the National Health Service, and the private health care providers that exist in the US and the UK. Due to the competitive nature of the market for health care in the US, maximising supply should not be the priority, otherwise you may end up with an excess of supply over demand for health care – hardly an efficient allocation of resources. Instead, ensuring effective resource allocation subject to the demand and supply for health care should be the primary role for the competitive market for health care in the US.
Imperfect competition, in the form of oligopolies and asymmetric information, in the health care industry in the US, however, causes the role of the markets to be distorted often resulting in market failures such as niche markets and market segmentation (Grembowski, Diehr, & Novak, 2000). In addition, regulators should also intervene to eliminate these market failures, where possible, in the US health care system in an attempt to maximise the provision of health care to individuals.
In summary, the role of the regulators is to encourage the production of health care and the role of the markets is to allocation resources in the most efficient manner.
Conclusion
The demand for health care, when it is provided at no cost to consumers, exists at a maximum level. The supply of health care, provided by the government, is determined by a number of variables, including the costs of production and the level of funding received through taxation. When health care is provided at a positive cost consumers enter into contracts with insurance providers, this creates a situation where policy intervention becomes necessary to ensure all parties enjoy the benefits of information symmetry and properly defined contracts.
The UK model benefits from a service that is provided when needed and is not based on an individual’s ability to pay. The lack of a profit-maximising incentive within the institutions providing health care results in aid provided primarily to heal the injured rather than efficient operation becoming more important than the quality of service. However, because prices play little role in incentivising agents, inefficiencies can occur in the UK system of health care provision and is the main disadvantage of the model.
The competitive market for health care in the US means that the provided level of health care is likely to be closer to the socially optimal level of provision given the demand and supply for health care. It is also a much more contestable market, with fewer monopolies, further increasing economic efficiency. However, the positive cost of health care creates the social and political issue of whether your access to health care should be a function of your disposable income.
Regulators’ role in health care markets should be to encourage the production of health care from the sub-optimal level initially provided in competitive markets, to the more efficient level. This is achieved by regulating firms’ costs and the minimization of them in order to maximize production. This is especially important in the UK market where output of health care is only a function of costs due to the lack of competition and the publicly-funded nature of the industry. The role of markets is to determine the largest provision of health care at the lowest cost possible; the most efficient allocation of resources given the demand and supply for health care. Markets and regulators work in conjunction to solve a problem with health care under competitive markets, that they are inefficiently supplied in less-than-optimal quantities.
Recommendations
Throughout the report, we saw the characteristics, positives as well as drawbacks from the two different healthcare systems, public and private funded. We also evaluated the importance of government interventions and the role of regulators in order to avoid market failure.
In the case of the UK system, a state-funded healthcare provision ensures equal services for all citizens and no regional monopolies. The system is also benefited from massive economy-of-scale and being an effective economical tool to keep the workforce at a healthy state. However, it suffers lack of innovation and development, leading to insufficient in quality and quantity of healthcare services in long-term. Resources allocative inefficiency and waste are also major problems for the UK market. Therefore, the role of the government and regulators here needs to be more decisive. There are different ways to minimize these disadvantages in long-term, such as:
- Increase the retirement age: Easing up the pressure from dependant population on the healthcare and insurance system.
- Provide more vacancies as well as training for part-time staffs in NHS facilities: Enable to satisfy a higher level of demand as well as improve the quality of services.
- Easing the immigration barriers for doctors from abroad: As high-skilled staff requires long time to train.
- Improve the qualities of appliances in existed NHS facilities: Other than building new ones.
- Encourage and subsidy researches: For low-price medicines, stem cell and gene technology.
- Organize campaign and informative programs: To educate people live, keep their family and surrounding environment healthy and hygiene.
As for the US, having a competitive market model helps the healthcare system become economic efficient, offer opportunities for business which stimulate innovation and technology development, and most importantly, avoid waste for both government and citizens. But, like the UK, the US system also has its own drawbacks. The provision of special treatments is not equally distributed for everyone, and the heavy reliance of Americans on the insurance system creates exploitation and domination of insurance companies. Though, economically, the US system is working well, it still requires government interventions to ensure social welfare and equality.
Read Also: Critical Analysis Nursing Care for the Older Adult


You must be logged in to post a comment.